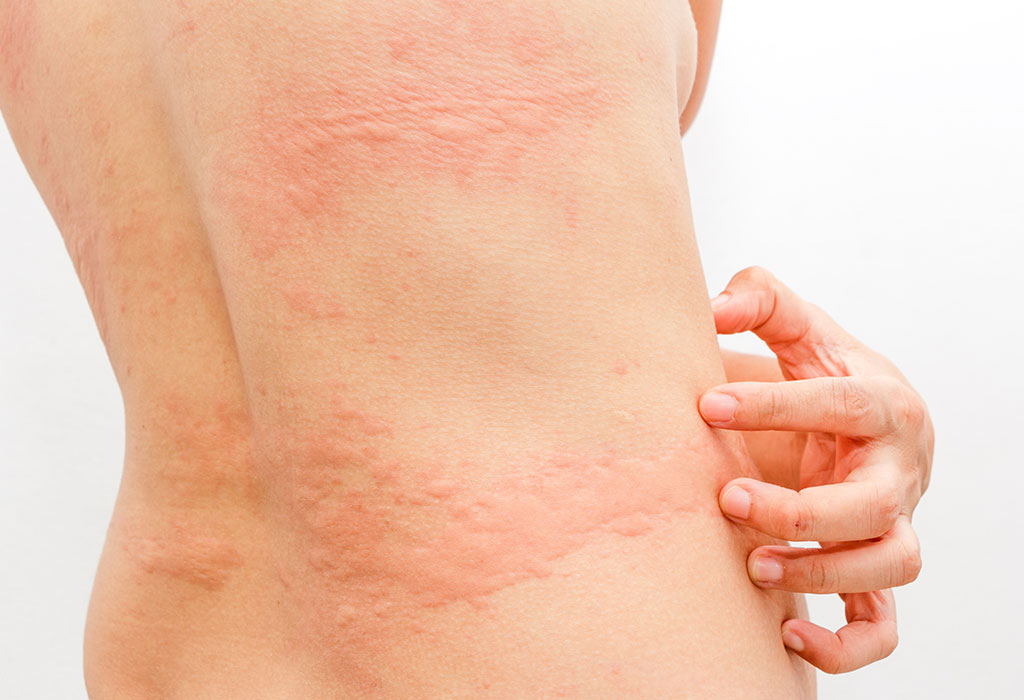
Postpartum hives or post-pregnancy rash, present as an itchy, bumpy skin rash, often appearing on the arms, back, and feet. Alternatively, it is also called welts, nettle rash, or wheels. As the name suggests, some women may experience these red or skin-colored, itchy rashes after giving birth, potentially due to allergic reactions or psychological factors such as severe stress. Other contributing factors include hormonal imbalances, infections, sluggish liver function, and changes in the immune system. It is important to note that postpartum rashes are not contagious. Although the duration of the rash can vary, it typically resolves with appropriate treatment over time. In the case of skin discomfort, consultation with healthcare professionals is vital.
Dermatology clinical trials conducted by clinical research organizations in the United States actively explore innovative therapies for various skin conditions, including postpartum hives. Participation in these clinical trials might serve as a gateway to personalized care and novel therapeutics.
Walk through the blog to educate yourself on the postpartum rash, conditions similar to a postpartum rash, the impact of hives on the pregnancy journey, and viable treatment options
What Does Postpartum Rash Look Like?
The skin texture and symptoms experienced by individuals with postpartum rashes, such as redness, itchiness, raised welts, or hives, resemble those of several skin conditions. Urticaria is one of the skin conditions with similar characteristics to postpartum rash, commonly known as hives. Urticaria is characterized by raised, itchy, and often red welts on the skin, which can vary in size and shape. Both postpartum rash and urticaria manifest itchiness and bumpy rashes, as they may share some common underlying causes, such as allergic reactions or stress.
However, it is essential to note that skin conditions can have various causes and manifestations. A healthcare professional’s evaluation is necessary to accurately diagnose and differentiate between specific skin conditions and determine the most appropriate treatment.
What Causes Postpartum Hives?
Postpartum hives are a post-pregnancy rash that affects women post-delivery. To be able to find relief from hives, the key is to track the triggers and seize control of them. Some of the commonly observed triggering factors are:
- Certain medications
- Foods (nuts, shellfish, eggs, dairy products, some fruits, and vegetables)
- An insect sting or bite
- Latex
- Pet dander, or plants and pollen
In response to the above-mentioned triggering factors, the body releases histamine, a chemical perceived by the body as a harmful substance. Consequently, the skin breaks out in itchy, red welts.
Other triggering factors lie under human control and should be regulated to avoid flares. These are as follows:
- Stress
- Overreaction to sweat, heat, or cold
- Sunlight
- Pressure on the skin
- Infection
- Medical treatment, such as a blood transfusion
- Smoking
- Eczema prone skin
Does Postpartum Hives Affect Face?
During pregnancy, it is not uncommon to experience skin changes from hormonal changes. About 1 in 150 women face a serious form of hives during pregnancy. A brief overview of skin variations during pregnancy is— acne, skin darkening, and stretch marks. Hives during pregnancy affect the face and other parts of the body. The areas commonly affected are:
- Chest
- Abdomen
- Back
- Upper arms
- Buttocks
- Upper legs
- Mucous membranes of the eyelids and mouth
Correlation Between Postpartum Hives and Breastfeeding?
In general, there is no direct cause-and-effect relationship between breastfeeding and postpartum hives. The hormonal influence of prolactin, a hormone essential for milk production post-pregnancy, is an allergic reaction as a skin rash/ hives.
Not all women who breastfeed experience postpartum hives, as many women successfully breastfeed without hives or skin issues. In case of breakout while breastfeeding, it’s essential to consult with a healthcare provider to determine the underlying cause and receive appropriate treatment or guidance.
Ways To Treat Postpartum Hives
Besides conventional medications, at-home remedies and preventive strategies also help alleviate the symptoms, allowing the mothers to share an intimate bond with their little ones without the fear of affecting them. In a few instances, a combined approach works best to curb the effects of hives.
-
Pharmacological Agents
- Over-the-counter (OTC) or prescription antihistamines
- Corticosteroids like prednisone
- Immune modulators
- Bromocriptine, a dopamine antagonist, for high prolactin levels
-
Preventive Measures
Amidst pregnancy, following some effective preventive measures does help relieve distress from skin conditions, including hives.
- Avoid extreme showers (too hot showers or hot baths)
- Avoid wearing tight clothing
- Try not to scratch the skin if it itches
- Keep pressure off the skin
- Avoid stress and practice relaxation techniques
-
Home Remedies
Every individual experiences a unique set of symptoms and responds differently to treatment regimens. A few women are effectively able to manage hives with at-home tips. These include:
- Applying cold compresses to the affected skin for 10–20 minutes or as needed
- Using anti-itch creams on the skin
- Avoiding scratching the hives
- Taking lukewarm baths with colloidal oatmeal
- Wearing loose, comfortable clothing made of 100% cotton
- Take a bath in lukewarm water and refrain from scrubbing the skin
- Using fragrance-free soaps, which are suitable for sensitive skin
- Tracking symptoms and identifying triggers
Conclusion:
The takeaway of this blog implies postpregnancy rash/ hives are a temporary pregnancy or post-pregnancy condition. The appearance and location of postpartum hives can vary from person to person. Some woman experience hives primarily on their arms, back, or feet. Others may have hives that affect the face, neck, or other areas. The distribution and severity of the hives depend on factors such as the underlying cause, individual sensitivity, and the immune system’s response. It is important to take notice of skin issues and consult derma specialists for help. Another alternative is participation in dermatological clinical trials to access novel therapies under investigation.